The term ‘prostatitis’ will be used to refer to chronic prostatitis (as opposed to acute prostatitis).
Although prostatitis is a common condition in men, it remains a largely neglected and poorly managed medical problem. The outcomes of traditional treatments for prostatitis, such as oral antibiotics, remain disappointing.
About 50% of patients who have a comprehensive men’s health check at this clinic have one or more of the manifestations of prostatitis listed below.

What are the common manifestations of prostatitis?
Pain or discomfort
Most commonly felt in one or more of the following areas:
- the perineum (the area between the scrotum and the anus).
- the penis (sometimes only felt in the tip of the penis).
- the testes.
- the groin.
- deep in the pelvis (‘chronic pelvic pain sydrome‘).
Sometimes the pain is triggered by or made worse by having an orgasm.
The severity of the pain varies from mild to severe, and often fluctuates over time. It can significantly affect a man’s quality of life.
The role of MRI of the prostate in the diagnosis of men with chronic prostatitis and chronic pelvic pain syndrome is currently being evaluated.
Urinary symptoms (sometimes referred to as ‘LUTS’)
Prostatitis can cause a wide spectrum of urination problems. They include:
- Urinary frequency or urgency, or getting up at night to urinate.
- Burning when passing urine.
- Reduced urine flow.
- Finding it more difficult to initiate urination.
- A discharge from the tip of the penis (sometimes).
Fluctuating PSA
The blood level of PSA (prostate-specific antigen) is often used to screen for prostate cancer.
Fluctuating PSA is a common manifestation of prostatitis, and often causes concern that prostate cancer may be present. When prostatitis is present, the PSA tends to rise, and then down go down again over a 12-month period.
Many men with fluctuating PSA caused by prostatitis are frequently referred to a urologist repeatedly over the years, with the aim of looking for prostate cancer every time the PSA rises again.
‘Silent’ prostatitis
The only indication that prostatitis may be present is finding a few red and white blood cells in a standard urine test. Further urine and semen testing can often confirm the presence of prostatitis.
What are some of the longer-term consequences of prostatitis?
- Increased risk of developing prostate cancer in the future.
- Increased risk of male infertility, through ‘oxidative stress’ and sometimes the triggering of anti-sperm antibodies (ASAB).
What are the causes of prostatitis?
1. Infection
Men with this form of chronic prostatitis have no obvious signs of infection such as fever.
The infection is most commonly caused by bacteria. Other microorganisms (for example viruses) are sometimes involved. It is very likely that some of the causative microorganisms can’t be detected by current testing methods.
How the infection occurs in the first place remains the subject of much debate. In some men however the infection is sexually-transmitted.
2. Inflammation in the absence of infection
In this second group of patients, there is inflammation in the prostate without infection.
For men in this group, it is thought prostatitis was initially caused by an infection, which then subsequently resolved spontaneously. The initial inflammatory process triggered by the infection then either self-perpetuates, or inflammation elsewhere in the body continues to drive the symptoms of prostatitis (See ‘Chronic gut symptoms below’).
In addition to the two main causes of prostatitis outlined above, there are often other important factors present which predispose to the onset or on-going symptoms of prostatitis and chronic pelvic pain:
- Changes in the pelvic floor muscles
These can occur for example after prolonged periods of sitting, or from lower back problems. - Chronic gut symptoms
The observation that chronic prostatitis and ‘IBS’ are often associated had already been made many years ago. - Some nutritional deficiencies (zinc, magnesium and vitamin D play an important role in prostate and pelvic floor health).
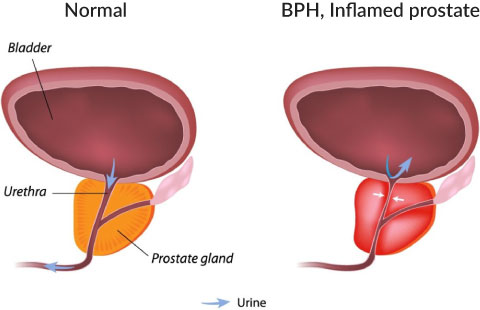
- It is likely that in some men, an enlarged prostate (BPH – benigh prostatic hyperplasia) may also play a role.
What treatments are available for prostatitis?
Prostatitis is often routinely treated with a course of antibiotics (generally 2 to 4 weeks) even when no specific bacteria have been isolated. This approach is therefore ineffective in most men, with symptoms either not improving or recurring weeks or even months after the end of the treatment.
Addressing both the causes and predisposing factors of prostatitis is key to a successful outcome. In my practice therefore I implement a combination of treatment approaches, each tailored to the individual patient’s situation. In most men, only three or four of the treatment approaches listed below will need to be considered.
- Acoustic wave therapy/shockwave therapy (SWT):
This treatment approach has several important beneficial effects: it increases blood flow in the prostate, directly reduces pain or discomfort, and causes muscle relaxation. Increasing blood flow improves delivery of anti-bacterial and supplements to the tissues of the prostate. - Supplementation to support the nutritional requirements of the prostate (for example zinc).
- Non-pharmaceutical antibacterial and anti-inflammatory compounds.
- Medicines to improve urinary symptoms and increase blood flow to the prostate.
- Management of chronic gut symptoms (‘IBS’ or other):
If present, it is important to consider whether these may be driving on-going symptoms of prostatitis. I believe I am the first physician in Australia to proactively treat both conditions in men presenting with prostatitis and chronic gut symptoms (see ‘Gut microbiome’). - Management of pelvic floor problems:
These two broad conditions can contribute to or amplify the symptoms of prostatitis.
I work in close collaboration with a physiotherapist who specialises in the management of pelvic floor dysfunction in men. - Assessment and management of ‘Mind-Body’ factors:
In any situation where symptoms have been present for a long time, the role of the mind in contributing to the on-going symptoms of prostatitis must be considered and addressed. - Antibiotics:
I avoid using antibiotics wherever possible. They can however be considered when a specific bacteria has been isolated and its sensitivity and resistance status clearly established.Antibiotics however have only poor penetration into the prostate tissues, and it is therefore important to combine them with one or more of the other treatment modalities listed above.
Acoustic wave therapy or Shockwave therapy (SWT)
What is the treatment protocol for Shockwave therapy for chronic prostatitis?
There are four treatment sessions, with a 1-week interval between each session. Each session lasts about 30-40 minutes.
Who will deliver the shockwave therapy treatment?
Men’s health physician – Dr Rob King himself will be giving the Shockwave therapy treatment. This ensures the best possible outcome for the patient.
Is the treatment painful?
The different settings for the delivery of the sound waves are adjusted for each individual patient. This ensures the intensity of the treatment is below the patient’s pain threshold.
What is the cost of Shockwave Therapy for chronic prostatitis?
The total cost for the four Shockwave Therapy treatment sessions is $2800.
Please note that this cost does not include the initial assessment consultation with Dr Rob King. This important initial assessment will determine whether you are likely to benefit from Shockwave therapy, and which treatment combination will best suit your personal situation (See ‘What treatments are available for prostatitis’ above).
The total Medicare refund for the four sessions is $422. If you have reached the Medicare safety net, then the refund is 80% of the total cost. Please note that private health funds do not at this stage cover any of the cost of the treatment.
How do I get started?
All bookings must be made online through this website. You will first need to register, a quick and easy process. All the demographic data you enter will be used to prepare your medical record prior to your first consultation. You can then book your appointment, selecting the ‘New patient appointment’ option.
